Let Dentrix attach images to claims whenever it can, or notify you that an attachment is required by the insurance company if it cannot attach the files automatically.
Updated 10/20/21
It’s always a challenging part of a dental office manager’s job to get dental insurance companies to pay for procedures in a timely manner. Insurance companies will use any excuse to delay paying, and there’s often additional information and/or attachments that are required for certain procedures to get them to process a claim.
With the constant changes in dental insurance, knowing what types of information are required for each insurance company and for each procedure code can be difficult to keep up with.
For eClaims customers, Dentrix G7.3 and higher includes a feature that will automatically attach images to claims whenever it can, or notify you that an attachment is required if it cannot attach the files automatically. Each insurance company can have its own attachment requirements, which can be entered and saved in Dentrix.
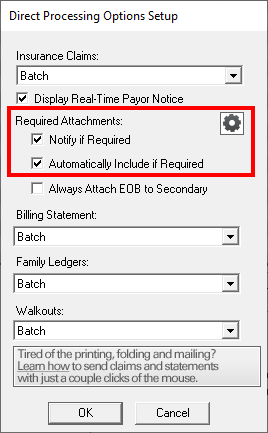
The Automatic eClaims Attachments feature can benefit your office in a couple of different ways.
You may have administrative team members that don’t have the experience to know exactly which types of attachments are needed for each procedure. Even with seasoned team members, constant changes in insurance requirements make it difficult to keep up with requirements.
Failing to provide required information to insurance companies can cause delays in payment. These delays can be significant. If a claim for a crown usually takes four to six weeks to be paid by insurance, and the necessary attachments aren’t provided when the claim is initially submitted, the insurance company can often take an additional four to six weeks once they receive the attachments to process and pay the claim. It’s best to provide the information when the claim is originally submitted to avoid these delays.
The Automatic eClaims Attachments feature eliminates the need for team members to have to remember which insurance company requires certain types of attachments for procedures by having automatic attachments set up by insurance company and by procedure code.
Having this information attach automatically ensures it is sent with the original claim, avoiding payment delays. Plus, you’ll save time by not having to add these attachments to claims manually.
As you discover other procedure codes that may require an attachment, you can customize and add attachment requirements based on the needs of your office and trends that you notice with the insurance companies you work with.
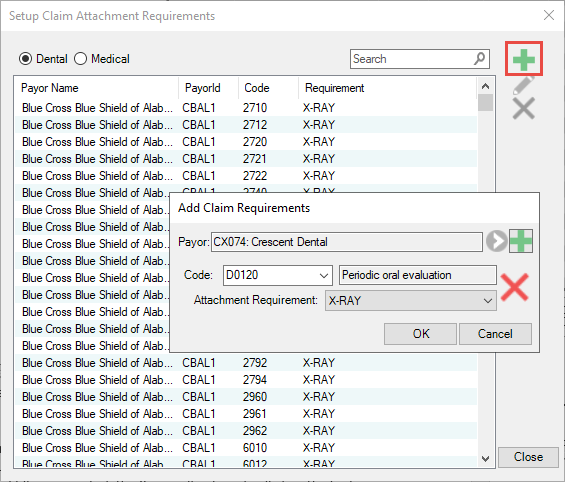
For example, I worked with an office recently that said they have to send an X-ray for an occlusal filling for a particular insurance company. It would be a good idea for them to add this information into Dentrix so that when a claim for an occlusal filling is created, the X-ray will automatically be attached.
Having Dentrix automatically add required attachments can save time by automating the process for you. It eliminates the need for team members to know the different types of attachments required by insurance companies, which may be very challenging, especially for newer employees. Most importantly, by automatically adding attachments, you’ll know all required attachments are sent with the initial claim to avoid delays in claim payment.
Learn More
For additional information, watch this video showing how the Automatic eClaims Attachments feature works.

By Charlotte Skaggs
Certified Dentrix Trainer and The Dentrix Office Manager columnist
Charlotte Skaggs is the founder of Vector Dental Consulting LLC, a practice management firm focused on taking offices to the next level. Charlotte co-owned and managed a successful dental practice with her husband for 17 years. She has a unique approach to consulting based on the perspective of a practice owner. Charlotte has been using Dentrix for over 20 years and is a certified Dentrix trainer. Contact Charlotte at [email protected].





